|
ENVI-HEALTH GROUP COMMENDS CITY RESOLUTION ON MED WASTE, RAISE CONCERN ON POSSIBLE MED WASTE INCINERATION REVIVAL
|
September 7, 2011
Environment health group, Health Care Without Harm-Southeast Asia (HCWH-SEA) today commends a city resolution under discussion in Puerto Princesa City Council that would ensure safe and proper disposal of medical, infectious and toxic medical waste. The resolution proposed by Councilor Miguel Cuaderno IV will use autoclave in the treatment of infectious medical wastes from hospitals, infirmaries, birthing homes, clinics, laboratories, drug manufacturers, institutions, mortuary and autopsy centers. “This resolution shows that what we need right now is the strict implementation of law through local ordinances,” said Merci Ferrer of HCWH-SEA. “Not revival of incinerators or promotion of incineration-in-disguise projects and waste-to-energy projects” after the collapse of a Baguio City dumpsite. In August 2010, HCWH-SEA together with other environment organizations dialogued with the Department of Health (DoH) after it obtained a copy of the Department’s Health Executive Agenda for Legislation (HEAL) proposing amendment to the Clean Air Act by re-allowing the use of incinerations. DoH immediately retracted the proposal. The group is concerned that the DoH would soon propose the use of medical waste incinerators to address wastes coming from the health care sector following recent announcements from the MMDA and Sen. Antonio Trillanes IV pushing for the use of incinerators to address the burgeoning waste problem in Metro Manila. “We would like to remind MMDA Chairman Atty. Francis Tolentino and Sen. Trillianes that there are safe and far more economical ways of minimizing wastes, treating and then disposing them properly without sacrificing the environment and the health of the people,” said Ferrer. |
“Time and again, we pushed for reduction-reuse-recycle when it comes to waste management both in households and health care system,” said Ferrer. “In hospitals for example, 90% of medical wastes when properly segregated are regular household wastes that maybe reused or recycled and composted. The remaining 10% infectious wastes are then handled using alternative waste treatment technologies such as autoclave and microwave.”
She added that hospitals around the country have proven that through proper waste management and the use of alternative waste treatment technologies, the volume of wastes have significantly decreased. The budget for managing the wastes has likewise decreased. In fact, through recycling and composting, these hospitals were able to raise additional income for their hospitals. “Incineration will not solve the garbage problem,” said Ferrer. “Without the basics of waste minimization and proper waste segregation, all wastes will end up being incinerated.” Incineration releases dioxins and furans, two of the most toxic and persistent pollutants known to science. “We are worsening the already grim situation of our garbage,” said Ferrer. “Zero toxin emission is a hoax.” The group is encouraging the health care sector to continue implementing proper waste management and to rally against possible medical and solid waste incineration revival. “The health care sector people know first-hand the ill-effects of incineration to health.” They are likewise encouraging local governments to follow the model of Puerto Princesa City in working towards proper waste management not just in the hospital but for the whole community |
Manila 2011 Declaration on Mercury-Free Healthcare

http://farm1.static.flickr.com/59/
Gathered in Manila, Philippines on the occasion of the Asia Regional Conference on Mercury-‐Free Health Care, more than 100 representatives of ministries of health and environment, health professional organizations, hospitals, and other health sector organizations from ten Asian countries came together to address policy and technical issues regarding the substitution of mercury-‐based medical devices.
The group made the following declaration:
Recognizing,
the important role the health sector plays in protecting and promoting public health;
the negative consequences of mercury pollution on human health; the negative impacts of mercury pollution on the environment; and mercury’s toxic, persistent and bioaccumulative nature;
Recognizing that,
alternatives to mercury-‐based medical devices are available, affordable and at least as accurate as mercury devices in their use; health systems in many countries in Asia have switched or are in the process of switching to the available alternatives;
the WHO-‐HCWH Global Initiative for Mercury-‐Free Health Care aims to substitute 70 percent of mercury thermometers and blood pressure devices globally by 2017; the substitution of mercury-‐based medical devices will contribute to health system strengthening by improving the quality of health care and the occupational health and safety of health care workers; the world’s governments are negotiating a legally binding treaty to phase-‐out most uses of mercury;
We, the participants in the Asia Regional Conference on Mercury Free Health Care recommend the following plan of action.
For Governments and Regional Bodies:
1. Formulate the policy and directives to phase-‐out the use of mercury devices in the health sector’s day-to-‐day practice.
2. Promote multi-‐sectoral collaboration for better implementation of policy-‐based plans, including
collaboration between Ministries of Health, Environment and Industry.
3. Provide information to the people—including health professionals-‐-‐ regarding the harmful effects of mercury, thereby educating and communicating with a diversity of stakeholders.
4. Replace mercury devices with alternatives that are at least as accurate and well calibrated as mercury
devices in public health facilities.
5. Identify not only alternatives to mercury-‐based medical devices, but also provide for the safe storage and disposal of these mercury devices—including potentially mandating extended producer responsibility.
6. Encourage the development of an appropriate plan for the phase-‐out of mercury thermometers and sphygmomanometers in the International Negotiating Committee to Prepare a Global Legally Binding Instrument on Mercury.
For WHO and other UN Agencies
1. Make technical assistance and expertise available to Governments and other health sector organizations
for mercury substitution and safe disposal.
2. Produce information, educational, and technical guidance materials.
3. Make resources available for the initiation of Mercury-‐free Health Care.
4. Encourage policy makers to work towards mercury-‐free health care.
For Civil Society Organizations:
1. Advocate for policies and practices that substitute mercury-‐based medical devices with safe, accurate,
affordable alternatives.
2. Change the public perception of the issue through educational activities.
3. Work as a watchdog for the implementation of government activities and policies.
4. Network with different stakeholders, government organizations and civil society organizations to see the
effective implementation.
5. Promote initiatives in the private sector health institutions, as well as with manufacturers for mercury
free health care.
For the Private Sector
1. Phase-‐out the production, sale and marketing of mercury-‐based medical devices.
2. Expand production and distribution of non-‐mercury devices, making quality and validated alternatives
available at affordable prices.
3. Provide for Extended Producer Responsibility by taking back phased-‐out mercury equipment and managing the mercury waste.
4. Support the goals of mercury-free health care.
Manila, the Philippines, March 15, 2011
Japan Solidarity Statement
We the participantsin the Asia Regional Conference on Mercury-Free Health Care, more than 100 representatives of ministries of health and environment, health professional organizations, hospitals, and other health sector organizations from ten Asian countries gathered in Manila, express our profound solidarity with our brothers and sisters in Japan at this moment of crisis.
As we have discussed issues of environmental health during these days, the unfolding crisis in Japan--the earthquake, tsunami and nuclear catastrophe—has been constantly on our minds, as the Japanese people have been constantly in our hearts. We stand with them in this traumatic moment of need, and continue to dream of a world free of all forms of pollution.
Health Care Without Harm is an international coalition of 473 organizations
in more than 50 countries, working to transform the health care sector so it
is no longer a source of harm to people and the environment.
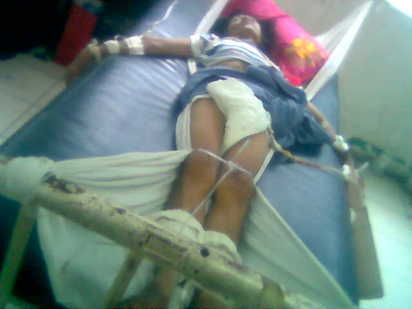
The Ties that Bind |
Medicine is an inexact science. It is constantly evolving making truths of today fallacies of tomorrow. The same is true with how medical science has approached theoretically and in practice mental illnesses. Throughout the centuries it has employed exorcism to asylums, bloodletting to lobotomy, from tonics to talk therapy with limited success. In the latter part of the past century, medical breakthroughs were discovered. Foremost of which is chlorpromazine which was prescribed to at least two million people within eight months of official release in 1954 and is still prescribed today. The same pattern of success was seen recently with the release of Prozac. It has achieved success even in pop culture with frequent reference to it in music and films. Some form of treatment appear strange and harrowing in the context of modernity's ease and convenience. Such is the case with lobotomy which consists of cutting the connections to and from, or simply destroying, the prefrontal cortex (the primary area where movement and memory are conceived and processed). Until the early 1990s, lobotomy was still performed in specialized psychosurgery centers in the United Kingdom for limited indications.(BMJ, 1996) These procedures often result in major personality changes and possible mental retardation. However, the most depraved form of "treatment" that has survived until now is the straightjacket. It is a garment shaped like a jacket with overlong sleeves. The ends of these can be tied to the back of the wearer, so that their arms are kept close to their chest with possibility of only little movement. It is used to restrain people who may otherwise cause harm to themselves and others. Restraints are also indicated for non-psychiatric use such as in orthopedic, geriatric, pediatric and post-operative care. For example, when a patient has a long-leg fracture, a restriction of movement may occur with the traction applied on the distal leg. The negative connotation of restraints dates back to the Victorian era wherein such method was employed as a form of torture. Straightjackets were considered before as more "humane" than other forms of bondage such as ropes or bolts and chains. Historically, the use of restraints has to do with the ignorance of the family of the patient and the people in the facilities that provide "care" to them. These patients are often left in poorhouses alongside criminals. They were thus bolted into prison cells. Surprisingly, such practices can still be seen in the Philippines and more visibly in Negros Occidental. When a family can no longer "control" a family member with a mental illness from his or her fits, they would usually get the assistance of the police. For the others who appear knowledgeable, they would call the emergency medical services. However, these medical service provider would call the police in stead fearing legal retribution and fearful of facing their own ignorance. If ever the patient gets restrained they would be left to the "care" of the police until formal medical care can be given--which means on the usual office hours or when the price is right. Unfortunately, there is no facility in the province that is specialized for such care. The lone facility that has semblance of it is provided by the Bacolod City government that gives fluctuating support. In that facility, psychiatric patients are also incarcerated while others are heavily sedated. The traditional straightjacket may not be visible (probably owing to lack of funds to purchase materials for it). In lieu of the jacket would be straps, cords and ropes that are tied on the patient's wrists and ankles. At the back of the Corazon Locsin Montelibano Memorial Regional Hospital a building was built around ten years ago but has never been used for such purpose. This might be due to lack of personnel (such as nurses) to work there. The psychiatric patients are in stead placed in the regular medical ward. Consequentially, they receive the same level of treatment and the same level of inattention as the other patients. The room delegated for such purpose is actually dangerous for the patient, hospital personnel and the public. The patients can climb the wall and break the glass window pane and use the sliver as weapon. The apparent danger they pose is meted with crude attention by the nurses and allowed by the doctors through restraints. Restraints can pose danger to the patients as well. Wearing an institutional straitjacket for long periods of time can be quite painful. Blood tends to pool in the elbows, where swelling may then occur. The hands may become numb from lack of proper circulation, and due to bone and muscle stiffness the upper arms and shoulders may experience excruciating pain. Thrashing around while in a straitjacket is a common, but mostly ineffective, method of attempting to move and stretch the arms. Other complications may be expected. Severe sensory deprivation can cause hallucinations and delusions. (Kenna, Hebb, et al, ) Apparently the same symptoms experienced by these patients are the same as those experienced by prisoners in solitary confinement, lone sailors and Arctic explorers. The Citizen's Commission of Human Rights (CCHR) have investigated and documented since 1969 deaths that occur with patient's under the psychiatrists' "care". It has documented 100 unexplained deaths in California's Camarillo and Metropolitan State Hospital. Along with that CCHR has exposed to the public that up to 150 restraint deaths occur every year in America alone. (Milken, 1998) Local data is not available. The CCHR argued that patients are provoked in order for restraints to be justified thereby giving the facility at least $1000/day from insurances. Unfortunately (or fortunately), the Philippine Health Insurance Corporation and most health insurances do not reimburse for psychiatric cases.The CCHR also noted that some patients on restraints get so exhausted while under sedative medications that they succumb to respiratory and cardiac arrests. Explicit policies and clear guidelines were usually deficient in psychiatric facilities. It is evident, however, that restriction of freedom is the only certain way of ensuring the safety of the patient and other persons in the vicinity, when that patient is violent and alternative methods of management have failed or have been rejected by the patient. Patients who are terrified by the feeling of loss of self-control, and patients who deteriorate in the over-stimulating atmosphere of the ward, may even request seclusion. Alternative methods to restraint can be the following: 1. Orders that the patient may not leave the ward without a chaperone and requiring the patient to remain in sleeping attire, thus limiting mobility. 2. Use of quiet rooms: Disturbed patients who are rapidly losing control may be requested to remain in a quiet room until their self-control improves. 3. Chemical restraints: Modern psychotropic drugs have been used for patients who need help in controlling their aggressive behaviour. It is often sufficient and possible to persuade the patient to ingest medication or take an injection voluntarily. As Jan Eastgate of CCHR puts it: It may be stating the obvious that psychiatric "care" is not supposed to kill patients, and certainly no one expects patients to die in psychiatric hospitals. yet this is what happens under the watchful eye of psychiatrists around the world. Psychiatric restraint procedures are "assault and battery", in every respect, except one; they are lawful. And because of this thousands of individuals die each year. It should be recognized by every hospital employees that psychiatric patients are entitled to the same rights and responsibilities as patients in any other medical setting. The facility should provide ample support to the patient and provide privileges that reflect concern for the patient's safety, well-being and increasing ability to be self-reliant and self-controlled. The institution should also formulate a written policy regarding the use of methods of limiting patients' freedom. This policy should be made known to all members of the hospital staff. The members and staff should then be aware and mindful of their responsibilities. Orders and records should be periodically reviewed in order to ensure that policies are followed. Chemical restraints should be given more preference over physical restraints owing to the latter's deep psychological impact and stigma. Understandably straightjackets are not products of the psychiatric patient's minds but borne out of the constricted, not-so straight minds of the public and medical "professionals". 1. Norway compensates lobotomy victims.British Medical Journal.1996;313:708. 2. Milken, D. Death By Restraint. Canadian Medical Association Journal. June 1998. 3. Kenna JC. Sensory deprivation phenomena: Critical Review and Explanation Models.Royal Society of Medicine.1962. 3. Citizens Commission on Human Rights. Deadly Restraints: Psychiatry's Deadly Assault. 2004. |
MMR Vaccine and Autism Link Debunked by Authorities
|
The association between Autism and the Measles, Mumps and Rubella vaccine was recently debunked by health authorities worldwide. The link, first suggested in a study conducted by British surgeon, Andrew Wakefield and other researchers, gained media attention when it was published by The Lancet in 1998. According to their study behaviour symptoms characteristic of Autism was observed fourteen days after the MMR vaccination. Investigative reporter Brian Deere first publicized in 2004 stories that criticized the Wakefield findings. On the basis of Deer’s reports, the British General Medical Council convened in 2007. The GMC concluded that Wakefield was paid to conduct the study by lawyers who have clients with adversarial claims to manufacturers of MMR vaccines. On ethical grounds he was cited to have conducted a study without approval from the ethics board and subjected children into unnecessary procedures. Consequently, Wakefield along with his co-author was stripped of his medical license in the UK. The Lancet retracted the paper after the GMC made its conclusion out. In 2007, ten of Wakefield’s 12 co-authors retracted declaring "no causal link was established between (the) vaccine and autism, as the data were insufficient". Alarmingly, the MMR vaccination rate has dropped to 80% since its publication, well below the 90% coverage needed to provide immunity to all persons in a community. |